Fitness to drive in a patient with aortic stenosis
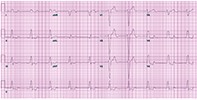
Margaret has been well known to you for years. She is an obese, independent 83-year-old woman who lives alone. Four years ago you performed a cardiac echocardiogram that showed she had moderate aortic stenosis. This was performed because she had an episode of mild congestive cardiac failure secondary to severe iron-deficiency anaemia. The anaemia was possibly due to gastrointestinal bleeding; it has not recurred and Margaret has refused all investigations since. She has severe renal failure (estimated glomerular filtration rate, 25 to 30 mL/min/1.73 m2) secondary to longstanding hypertension and she also has diet-controlled diabetes. For many years she has had a left bundle branch block on her ECG (Figure) but there is no other cardiac history.
Margaret is currently taking candesartan plus hydrochlorothiazide 16 mg/day, amlodipine 5 mg/day, ferrous sulfate one tablet twice a week, vitamin D 2000 IU/day and vitamin B12 injections every three months.
Margaret asks you to assess her fitness to drive for a routine renewal of her driving licence. You notice her ankles are swollen and her breathing is more laboured than normal. She denies any recent chest pain or shortness of breath. Due to her obesity, it is not possible to feel hepatomegaly.