Peer Reviewed
GP emergency management
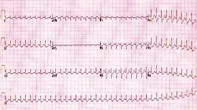
An older man with supraventricular tachycardia who has a cardiac arrest
Abstract
John, who is 78 years of age and is known to your solo practice, arrives for an 8 am appointment looking sweaty, grayish and agitated, and complaining of having had ‘palpitations’ since 5 am that morning. John is moderately overweight (body mass index, 29 kg/m2) and smokes 20 cigarettes a day. You have tried to get him to make lifestyle changes for several years, but he is not one for diet or exercise and he likes to drink red wine. He is usually hypertensive (165/102 mmHg) but he ‘isn’t good at taking the tablets’ you have prescribed. His last blood test was carried out in 2008 (despite your best efforts to encourage him to attend more frequently) and showed hypercholesterolaemia, hypertriglyceridaemia, probable fatty liver and a high normal blood glucose level.
Key Points
- Defibrillation requires some sort of myocardial electrical activity to be successful.
- Adrenaline should be used before defibrillation in cases of asystole, or when defibrillation does not result in a regular rhythm with effective cardiac output.
- Asystole or a pulseless idioventricular rhythm has a worse prognosis.
- When a patient is declared deceased, always consider organ donation possibilities when appropriate and whether or not the death could be a coroner’s case.
Purchase the PDF version of this article
Already a subscriber? Login here.